A pharyngoplasty is an operation to treat nasal speech. The decision to have this operation is made jointly by the patient / parent, speech therapist and surgeon.
How does this operation help?
The operation helps speech by stopping air escaping down the nose during speech. The impact on speech is noticeable immediately following the operation.
When we speak, air comes up from our lungs, through our voice box, and we then use our palate, tongue, lips and teeth to make the air into speech sounds. Most English speech sounds are produced through the mouth, so the back of the palate, which is the soft part, rises to close off the back of the nose so that the air is directed through the mouth (see Figure 1).
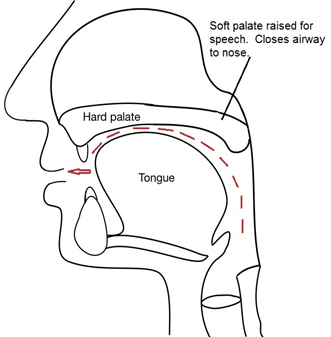
Figure 1: diagram showing how soft palate closes off back of nose, directing air to mouth for most speech sounds
For some people during speech the palate does not close off the back of the nose sufficiently (see Figure 2).
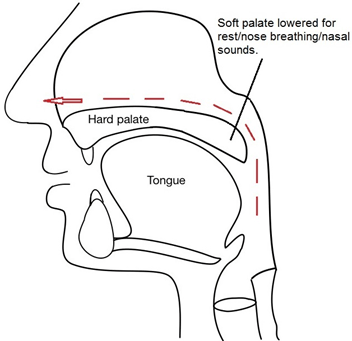
Figure 2: diagram showing how air can escape if soft palate does not close correctly
This may be for a variety of reasons, such as having:
- a repaired cleft palate
- a short palate in relation to the size of the throat, or
- a palate which does not move far enough or quickly enough.
What does the operation involve?
The operation is quite straightforward. During the operation, tissue at the back of the throat is rearranged to help the palate close completely.
This is carried out under a general anaesthetic. The patient will usually come into hospital the day of the operation and will need to stay in hospital for at least one night. The patient may have a sore throat for a few days and will need to eat a soft diet for a while, but advice will be given regarding this. Different people need different times to recover, but the patient will need to take some time off work or school following the operation.
Speech therapy alone will not help reduce nasal speech if the palate cannot move and close properly against the back of the throat. Sometimes speech therapy is needed after the operation to help learn a new, clearer way of speaking. Your speech therapist will discuss this with you.
Are there any risks / side effects?
As with all surgical procedures there are risks involved.
- One of the effects may be to make the speech sound as if the nose is blocked up, as if the patient has a cold. Also sleep patterns may be affected and there is an increased likelihood of snoring. Often these effects are more noticeable at first but wear off over time. If these effects do not wear off and are causing disrupted sleep or breathing the pharyngoplasty can be stretched or removed.
- Very rarely bleeding may occur following surgery, requiring urgent return to theatre. This occurs in fewer than 1 in 100 patients.
- There is also a small risk (less than 1 in 10 patients) of the wound breaking down as a result of infection. This may heal by itself. If not, another operation might be needed, usually several months later.
- Breathing through the nose may also be affected at first. This is because of the re-arranged tissue and the swelling caused by the operation. If this happens a small tube (known as a naso-pharyngeal airway) is put down the nose to help breathing for the first 24 to 48 hours after the operation. Fewer than 1 in 20 patients will require this.
The surgeon will discuss these risks with you before the operation.
4-6 weeks after surgery a review appointment will be offered at one of our clinics. A speech assessment will be carried out six months after surgery.